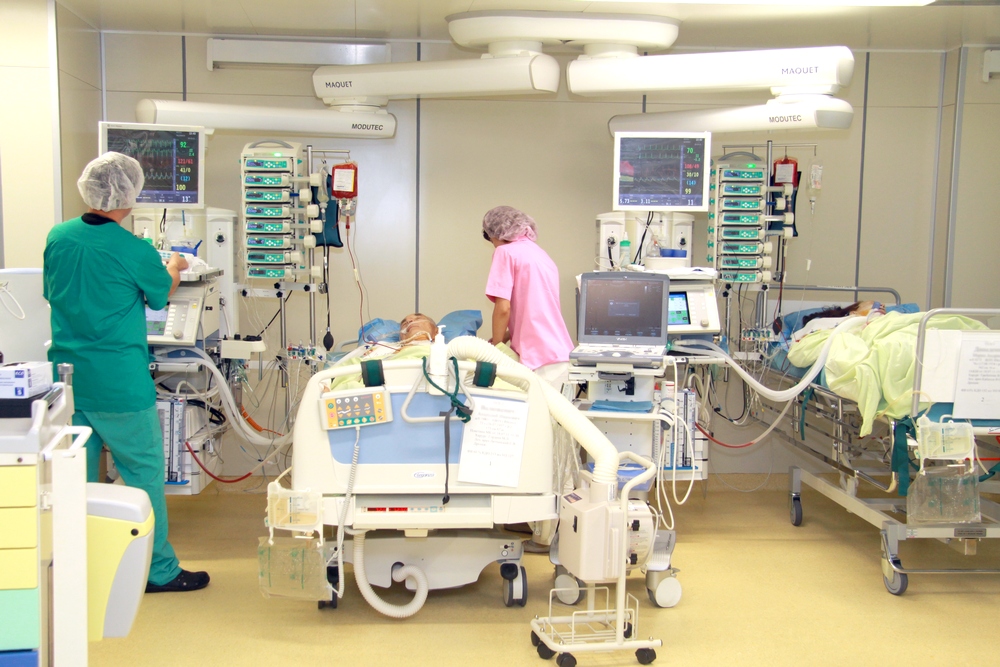
In May 2020, Almazov Centre, like most federal medical hospitals, was actively involved in providing care to COVID-19 patients. It should be noted that the tasks included not only the provision of a high-tech clinical service, which St. Petersburg urgently needed during the aggravated epidemiological situation, but also research support for COVID-19 response with the search for effective treatment methods.
The experience of our specialists has confirmed that the severe course of COVID-19 accounts for about 5% of cases. However, mortality in this form of the disease remains extremely high, reaching 80% in developed countries. This is mainly due to the multifactorial damage to the lungs and the body resulting from the direct pathogenic effect of the virus on the lungs, hyperimmune response to the infection and proven damage to the inner lining of blood vessels (endothelial dysfunction) with the development of thrombosis. In view of this, an effective treatment for severe COVID-19 should be comprehensive – it is necessary to impede the replication of the virus and damage to the lungs, interrupt the hyperactivity of inflammation and prevent increased blood clotting associated with endothelial dysfunction. The efforts of researchers and doctors have led to significant advances in the control of inflammation and the prevention of thrombosis. However, the first challenge of preventing viral replication and reducing the severity of lung damage is still far from being solved. Unfortunately, it should be noted that none of the many proposed methods has yet been acknowledged by evidence-based medicine.
One of the main mechanisms leading to severe lung damage in COVID-19 is the penetration of the virus into the alveolocytes (cells lining the lungs) with their subsequent death. The most important function of alveolocytes is the synthesis of pulmonary surfactant, which regulates the alveolar surface tension. In the absence of surfactant, surface tension increases and the alveoli collapse, causing impaired gas exchange and eventually fatal hypoxia. The aforementioned mechanisms of damage to alveolocytes and surfactant are typical of most viral pneumonia.
Surfactant-BL is an exogenous surfactant, which has been created and approved for medical use in Russia as a preparation being as close as possible in its chemical composition to the natural human surfactant. Almazov Centre has been using Surfactant-BL for ten years for the treatment of respiratory distress syndrome after cardiac surgery and for severe lung injuries of various origins, including pneumonia. Based on that previous experience and the positive results obtained in Russia during the swine flu pandemic, the technology of Surfactant-BL inhalation was used at Almazov Centre to treat 28 patients with severe COVID-19. Sixteen patients in infectious disease wards suffered from lung damage of 75 to 95% and severe gas exchange disorders, requiring transfer to the ICU. Surfactant inhalations resulted in an increase in oxygenation, relieved the shortness of breath and caused subjective improvement in condition. Only one case required transfer to the ICU. In 12 cases, inhalations of Surfactant-BL were used in patients with extremely severe COVID-19 treated in the ICU. To maintain gas exchange in these patients, modern methods of respiratory therapy were used, such as non-invasive lung ventilation and high-flow nasal oxygen inhalation. However, these measures were no longer sufficient, the need for ALV and intubation was considered. Surfactant administration made it possible to improve gas exchange, eliminate the need for tracheal intubation and ALV in 9 out of 12 patients. It should be noted that in addition to the reduced risk of transfer to the ICU and the use of mechanical ventilation, in this group of 28 patients with severe COVID-19, a significant decrease in mortality was noted, which was 14.3%.
The inhalation therapy with Surfactant-BL for severe forms of COVID-19 showed encouraging results in clinical centres in Moscow, Tyumen, Syktyvkar. According to colleagues, these early findings require in-depth follow-up, continued research and validation in large patient cohorts.
