Endometrial cancer is a malignant tumor that starts in the cells of the inner lining of the uterus. It is also called endometrial cancer, or endometrial adenocarcinoma.
Today, surgery for endometrial cancer is performed mainly laparoscopically (endovideosurgical method is used). The goal is to remove the tumor in order to further protect the patient from cancer recurrence. The uterus, cervix, ovaries, fallopian tubes are removed, and in some cases the iliac and para-aortic lymph nodes should be removed.
Based on the results of preoperative tests (uterine scraping, MRI, ultrasound), doctors determine the risk group of a particular patient and decide on the need for lymphadenectomy. Lymphadenectomy is definitely indicated at high risk and is not necessary at low risk, but at intermediate risk, the situation is ambiguous.
“From my experience, I can say that preoperative diagnosis is not 100% accurate. Even if a woman is considered to be at low risk according to her results, after surgical treatment and a histological examination of the removed tissue it may turn out that the risk was high and it was necessary to remove the lymph nodes. The patient will have to undergo a repeated surgical intervention with additional radiation therapy. But it may be the other way around, after a maximum removal it turns out that there are no metastases in the needlessly removed lymph nodes,” explains Professor Elena Ulrich, Head of Oncogynecology Research Laboratory of the World-Class Research Centre for Personalized Medicine.
Complete lymph node removal is a way to get rid of cancer, but at the same time such an intervention has serious consequences. Patients after lymphadenectomy suffer from lymphocysts and lymphostasis of the lower extremities (lymphedema, or elephantiasis, an abnormal accumulation of interstitial fluid, which occurs due to impaired lymphatic transport and causes an increase in the volume of the affected organ). These conditions are very difficult to treat, and patients will have to suffer from these complications for life.
Today, there are modern technologies allowing for an accurate intraoperative detection of the affected lymph node. Russian guidelines for endometrial cancer treatment include a method for sentinel lymph node detection.
In endometrial cancer, it is possible to intraoperatively identify the affected sentinel lymph nodes. They are removed because they are the first location being invaded by cancer cells. As the surgeons continue the surgery, the removed material is sent for urgent histological examination, and if it is not affected, lymphadenectomy is not performed.
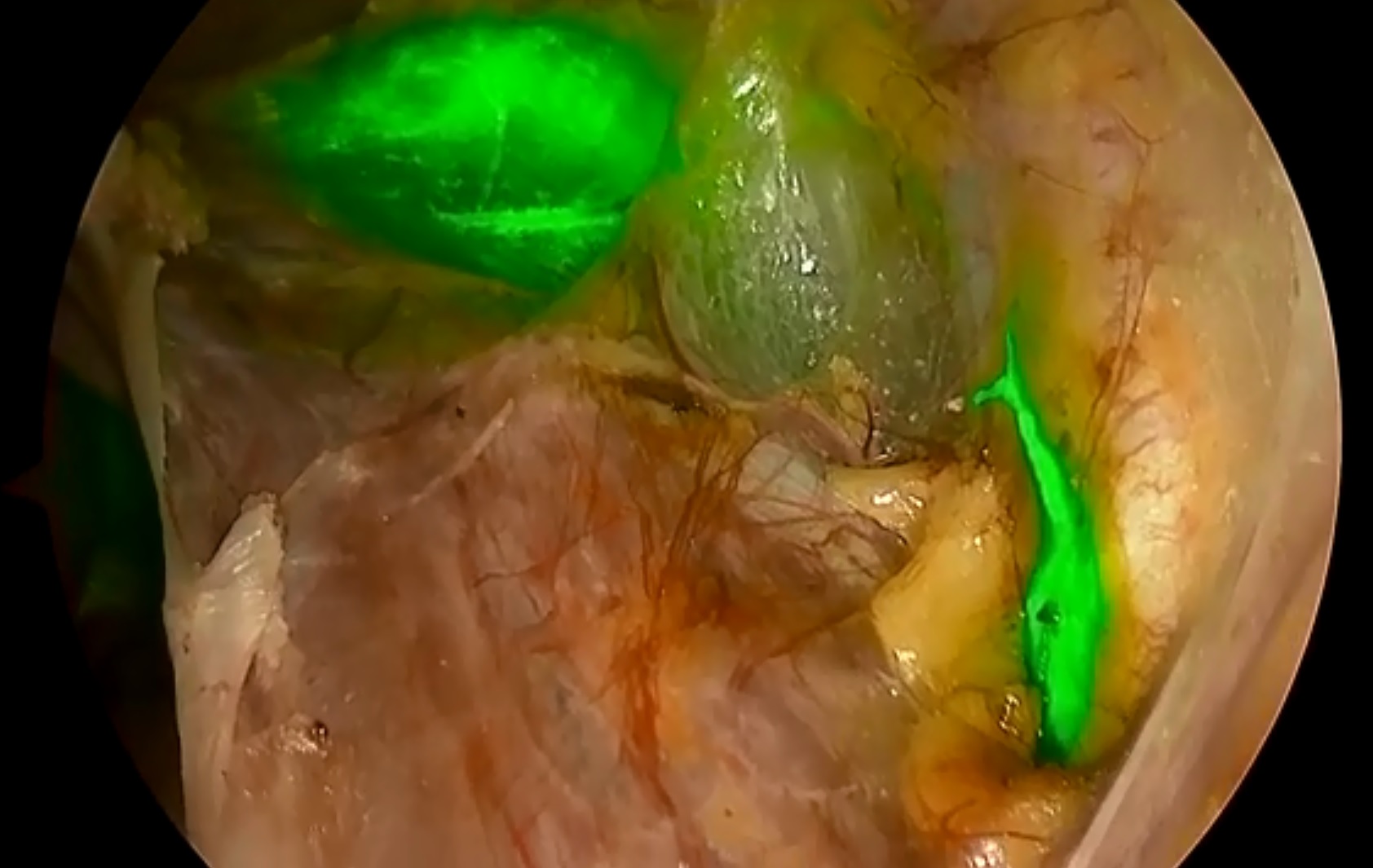
To map sentinel lymph nodes during a laparoscopic procedure, a special fluorescent dye indocyanine green is injected into the cervix, which in a few minutes accumulates in points where cancer cells are concentrated.
Then the operating surgeon sets up the optical mode (changes the spectrum of light that illuminates the operating field). In this special light mode, the affected lymph nodes that have accumulated the drug will glow green.
Endometrial cancer is commonly diagnosed in postmenopausal women – more than 90% of cases occur in women older than 50 years (the average age of patients is 65-69 years, the incidence among them being 98.1 per 100 thousand women). Under the age of 49, endometrial cancer is relatively rare (in 4-5% of all cases). Often, patients with endometrial cancer have a number of serious comorbidities: cardiac and endocrine disorders, etc. Due to these concomitant conditions such patients cannot be operated on in specialized cancer treatment centres, since they do not have additional services and specialists.
Almazov Centre is a highly specialized multidisciplinary medical centre where a multidisciplinary approach is offered to each patient. This means that doctors from different specialties: gynecologists, oncologists, cardiologists, endocrinologists and many others work together to develop a single tactic for patient management.
